Healthcare Practice Leader Laura Poltronieri, AIA, a principal in HOK’s Philadelphia studio, has dedicated her career to the design of healthcare environments for women and children. One of her sub specializations is the design of neonatal intensive care units (NICUs). In this Q+A, Poltronieri describes trends shaping the design of ideal NICU environments.
What is your favorite part of designing neonatal intensive care units?
The NICU clinicians and administrators who we have the privilege to work with are incredible individuals who have committed their lives to helping seriously ill infants and their families. I enjoy working with clinicians to envision and improve upon the ideal NICU environment.
We’re also thinking about how to use design to foster and empower relationships among clinicians, patients and families. Our planning process enables open communication that leads to compassionate, empathetic design. It’s through honest conversations with clinicians and patients that we can understand what the ideal environment looks like for mothers, newborns and clinical staff.
What are the benefits of NICU family couplet rooms?
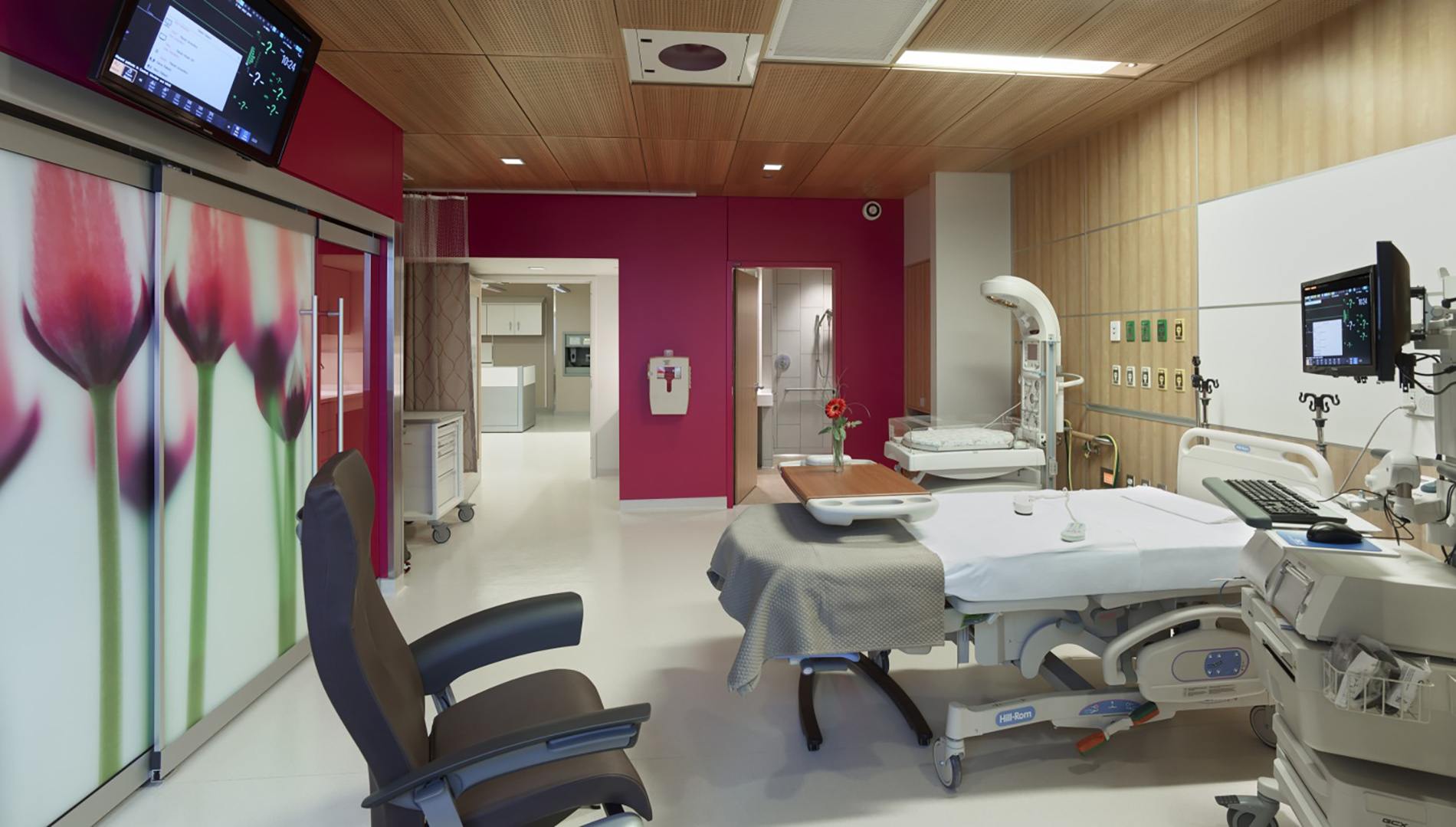
NICU family couplet rooms continue to grow in popularity as we bring a NICU level baby and postpartum mother into one room to receive care simultaneously.
In a traditional model, a new mother would be an inpatient on a postpartum unit recovering from her delivery and, if required, her baby would receive care in the NICU—often on a different floor.
With an integrated and redesigned unit, the mother and baby can now be cared for simultaneously in the same room. Once the postpartum mother is discharged, NICU babies can be transferred to private rooms that have accommodations for mothers to stay overnight as visitors.
Research shows that NICU babies who have close and regular physical contact with their mothers grow quicker, regulate their breathing and temperatures faster, and ultimately spend less time in the NICU. Parents also report that the more time they spend caring for their babies in the NICU, the more competent they feel when their baby is discharged and they go home.
How can NICUs support babies who don’t have mothers who visit regularly?
Clinicians estimate that approximately 20 percent of babies in the NICU don’t have family members who visit them on a regular basis. Knowing the importance of sensory stimulation for growth and development, hospitals are implementing robust complementary therapy and volunteer programs that connect volunteers with NICU babies. The therapists and volunteers support and supplement the babies’ health with programs including music and physical therapy.
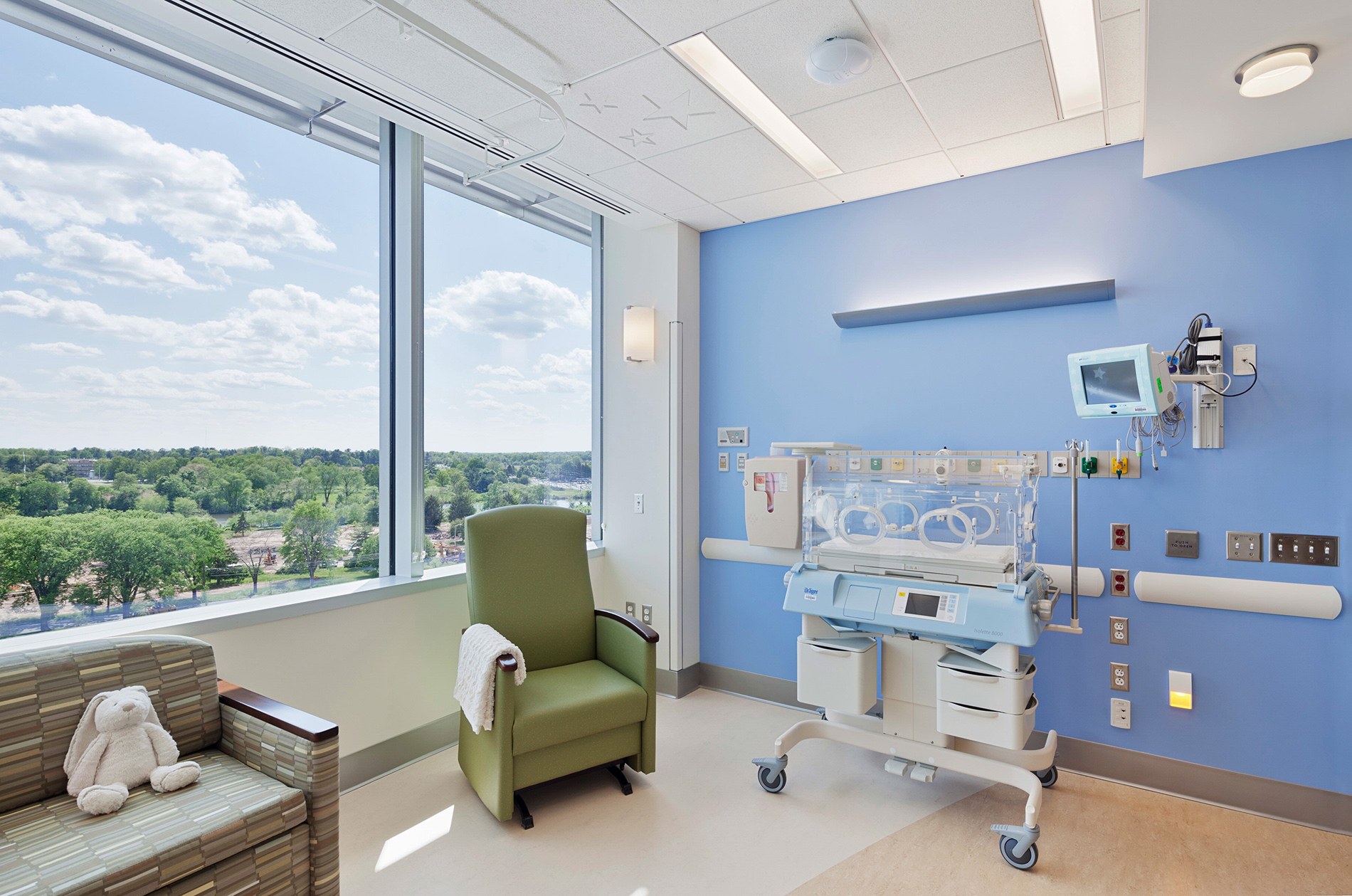
How do you address acoustics in NICU environments?
One could argue that the current concern regarding sound levels and the acoustic environments in hospitals began in the NICU. In fact, the “Recommended Standards for Newborn ICU Design,” originally published in 1976, was one of the first publications to implement specific acoustic targets for the NICU environment.
Since then, the impact of the acoustic environment on stress and sleep quality has become a major area of focus in broader hospital planning and design. Integrating sound monitors into NICU headwalls, selecting appropriate floor and ceiling finishes, and designing rooms that allow for the stocking of supplies and removal of waste without staff entering keeps sound levels to a minimum. Handheld monitoring devices for nursing staff can minimize audible alarms while ensuring that caregivers are alerted to any emergency.
How do you design for infection prevention in these spaces?
NICUs have always been at the forefront of infection prevention protocols with proactive and strict policies to ensure those who interact with patients are healthy, have their flu shots and are up to date on immunizations. This is especially important with low birth weight newborns in the NICU, who are more vulnerable.
There is also the added challenge of not wanting to severely limit visits from family members including siblings. Private and couplet rooms help contain the spread of infection. This is a continued impetus for moving to private patient rooms in NICUs.
Are there other trends impacting clinicians and patients?
We’re seeing the installation of infant-specific MRI equipment into NICUs at some of the leading academic medical centers. These compact machines support advanced neurological research studies that will ultimately help clinicians better understand the short- and long-term consequences of babies born prematurely with very low birth weights.
Simulation suites are also becoming integral to the design of NICUs, as they provide space for staff to keep up to date on training for how to respond to emergency situations.